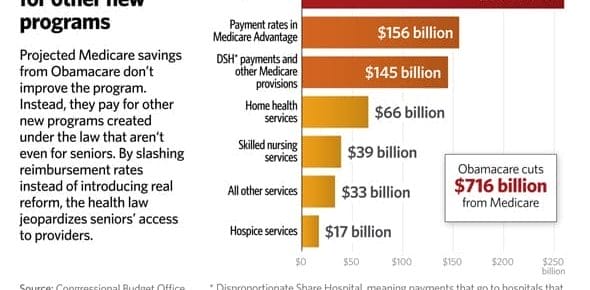
Many are surprised to learn that Medicare does NOT pay for a nursing home in most situations. Medicaid, not Medicare is the primary payer for most Georgia nursing home care. Medicare may cover the …
Continue Reading about Does Medicare Pay For A Nursing Home? →